How Long Can You Live With a Fatty Liver
- Research article
- Open Access
- Published:
Long term follow-upward and liver-related death rate in patients with non-alcoholic and alcoholic related fatty liver illness
BMC Gastroenterology volume xiv, Commodity number:166 (2014) Cite this article
Abstruse
Groundwork
Few studies accept compared the prognosis and liver-related mortality in patients with NAFLD (nonalcoholic fatty liver affliction) and AFLD (alcoholic fatty liver disease). We aimed to investigate the etiology and liver-related mortality of patients with liver biopsy verified fat liver affliction in a population based setting.
Methods
In this retrospective study, all patients who underwent a liver biopsy 1984–2009 at the National Academy Infirmary of Republic of iceland were identified through a computerized pathological database with the lawmaking for fatty liver. Only patients with NAFLD and AFLD were included and medical records reviewed. The patients were linked to the Hospital Discharge Register, the Causes of Expiry Registry and Eye for Addiction Medicine.
Results
A total of 151 had NAFLD and 94 AFLD with median survival of 24 years and 20 years, respectively (p = NS). A total of x/151 (vii%) patients developed cirrhosis in the NAFLD group and 19/94 (20%) in AFLD group (p = 0.03). The most common cause of death in the NAFLD grouping was cardiovascular illness (48%). Liver affliction was the most mutual crusade of death in the AFLD grouping (36%), whereas liver-related decease occurred in seven% of the NAFLD group. The mean liver-related expiry rate amongst the full general population during the written report period was 0.one% of all deaths. There was a significantly worse survival for patients in the AFLD group compared to the NAFLD grouping subsequently adjusting for gender, agenda yr of diagnosis and age at diagnosis (60 minutes 2.xvi, p = 0.009). The survival for patients with moderate to astringent fibrosis was significantly worse than for patients with mild fibrosis subsequently adjusting for gender, calendar year of diagnosis and historic period at diagnosis (60 minutes ii.09, p = 0.01).
Conclusions
Patients with fatty liver illness showed a markedly college adventure of developing liver-related death compared to the general population. The AFLD group had higher liver-related mortality and had a worse survival than the NAFLD group. Patients with more astringent fibrosis at baseline showed a worse survival than patients with none or mild fibrosis at baseline.
Groundwork
Fatty liver disease is clinically categorized into two chief groups, alcoholic fatty liver disease (AFLD) and non-alcoholic fat liver disease (NAFLD). NAFLD is condign i of the most mutual liver diseases worldwide [1] with a prevalence up to 30% in the general population [two] and it tin can progress to cease-stage liver disease [3]. NAFLD is associated with insulin resistance, and has been considered to be the hepatic component of the metabolic syndrome [3–5]. Patients with NAFLD have been shown to have increased cardiovascular mortality compared to the general population [6, 7]. Only a few studies take assessed the prognosis and take chances of liver-related expiry in patients with biopsy verified NAFLD in a population based setting [half-dozen, seven]. Thus, even though NAFLD is potentially a serious condition well designed population based studies on its natural history are lacking. Most recent studies on fatty liver disease have focused on NAFLD although AFLD is an of import crusade of fatty liver and just a few studies take compared the long term prognosis between NAFLD and AFLD [8–x].
The aims of this study were one) to examine the natural history and effect of patients with fatty liver disease with non-alcoholic and alcoholic etiologies. 2) Compare the prognosis and liver-related mortality in patients with NAFLD and AFLD, and compare these patients to the liver-related mortality in the general population. Our hypothesis was that these patients suffer from increased liver-related morbidity compared to the general population.
Methods
Population and instance finding
In this retrospective written report, a search was undertaken in a computerized diagnoses database from 1984 (when the pathology registry commenced their electronic registration) to 2009, in the Department of Pathology at the National University Hospital (NUH) of Iceland and identified all liver biopsies analysed and registrated in the SNOMED coding-arrangement, T-56000 and the M-50080 as having fat change. The SNOMED (Systemized Nomenclature of Medicine) is a coding system used in the pathology laboratories in Iceland to specify: Procedure, Topography, Morphology, Affliction and Etiology. This is a very valuable coding system for retrieving information and pathology reports from past years, similar biopsies of the liver (T-56…) showing fatty change (M-50080).
The catchment area of the NUH covers >95% of the population in Iceland.
All medical records from these patients were examined with respect to the following exclusion criteria: 1) presence of astute or chronic liver illness: PBC, autoimmune hepatitis, alfa-i-antitrypsin deficiency, hemochromatosis and viral hepatitis. 2) jejunoileal bypass performance. 3) employ of drugs known to be associated with fatty liver disease such as methotrexate, amiodarone, tamoxifen and high doses of corticosteroids. 4) malignancy at the time of index liver biopsy. 5) age nether eighteen years at the fourth dimension of index liver biopsy. half dozen) gallstone surgery at the fourth dimension of alphabetize liver biopsy. The patients with gallstone surgery at the fourth dimension of index liver biopsy were excluded to better represent the patients who would undergo a liver biopsy in clinical practise and non just the incidental finding of fatty liver during an operation.Indications for the index biopsy in the cohort were elevated liver tests, mainly serum alanine aminotransferase (ALT) and serum aspartate aminotransferase (AST) and/or hepatomegaly or suspected alcoholic liver disease. A total of 420 patients met the inclusion criteria and were divided into 2 groups, non-alcoholic and alcoholic group respectively (Figure 1).
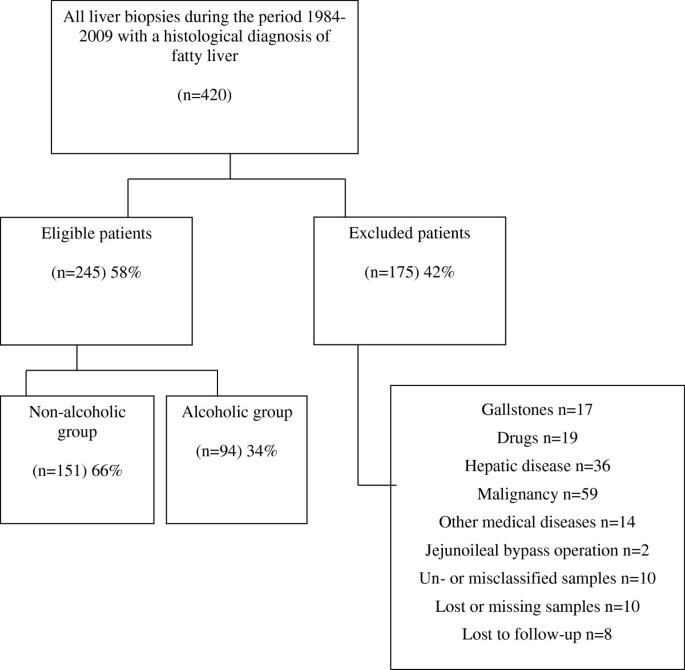
Flowchart of the patients. Reasons for exclusion from the written report are shown.
Data drove
The following data was obtained from the medical records and recorded at baseline: gender, age at diagnosis, height, weight and trunk mass index (BMI), history of diabetes mellitus, hyperlipidemia, hypertension, cardio- and cerebrovascular disease, liver disease and malignancy. Data on drug and alcohol intake was noted in the medical records. Patient with a reported booze trouble or abuse or an alcohol-related diagnosis before or at the time of liver index biopsy were considered to have alcoholic fatty liver disease. The diagnosis of cirrhosis was accepted in patients who had a discharge diagnosis, a death certificate diagnosis and/or histological confirmation in the follow-upwards period indicating cirrhosis. Laboratory data included at baseline were: AST, ALT, bilirubin, albumin, alkaline phosphatase (ALP), prothrombin time (PT), glucose, platelets count (PLT), serum cholesterol, serum triglycerides (TG) and mean corpuscular book (MCV). The last follow-up date was the 30th of November 2011.
Follow-up
All members of the cohort were linked through their unique personal identification number to the centralized Hospital Discharge Register at the Directorate of Wellness and the Registry of Causes of Death (RCD) at Statistics Iceland. Data was obtained from National Centre of Addiction Medicine in Iceland on whether or non the patients had undergone addiction therapy before or afterwards the fourth dimension of the index liver biopsy. This data was obtained from the addiction eye without knowledge of the liver biopsy results.
Patients were excluded if they were lost to follow-up in the registries. viii patients were lost to follow-up.
Upstanding considerations
The study was approved by the National Bioethics Commission (10-029-V1-S1) and the Icelandic Data Protection Authority (S4766/2010).
Histological nomenclature
The index liver biopsies were formalin stock-still and treated routinely in the pathology laboratory. They were paraffin embedded and cutting in 4–five micrometer thick sections. The sections were stained with hematoxylin and eosin, periodic acid Schiff reagent (PAS) with diastase and for reticulin. In addition a connective tissue stain, Weigert van Gieson or most unremarkably Masson Trichrome stain was performed. All histological slides were reviewed by experienced pathologists without knowledge of the clinical or biochemical information of the patients. Three pathologists (Jon G. Jonasson, David E. Kleiner and Sylvia O. Einarsdottir) divided the slides between them and reviewed all of the samples over a menstruation of ii years. The assessment was blinded to the clinical details. Second review to examine inter-observer variability was not undertaken. Morphological findings were recorded in a semi-quantitative manner regarding steatosis and fibrosis, which was initially proposed by Brunt et al. in 1999 and developed further by Kleiner et al. [11, 12]. Grade 0 steatosis was defined every bit < 5% fat and thus not compatible with fatty liver disease. Fibrosis stage were defined as follow: 0: none. i: Perisinusoidal or periportal fibrosis. 1A: balmy, zone 3, perisinusoidal. 1B: Moderate, zone 3, perisinusoidal. 1C: Portal/periportal. 2: Perisinusoidal, portal/periportal. 3: Bridging fibrosis. 4: Cirrhosis.
Statistical analysis
Statistical testing was performed using R-software. The results were presented as medians, interquartile range and range and as number (%). The Mann–Whitney U-test was used to exam for differences between groups. Dichotomous variables were compared by using the Chi-foursquare (X ii) or Fischer'south verbal test. A p-value of less than 0.05 was considered statistically significant. The survival curves were estimated past the Kaplan-Meier calculator, using years as the fourth dimension-scale and taking delayed entry into account. Differences betwixt groups were investigated by Wald test in Cox proportional hazards model, with age equally the fourth dimension-scale, adjusting for gender, calendar yr of diagnosis and age of diagnosis. The primary end-point was death from all causes.
Results
Overall 2262 liver biopsies were performed at the University Hospital of Republic of iceland during the written report period. A full of 420 patients with at least i index biopsy were identified past the computerized search in the pathology database as having fatty liver on biopsy. Those who were misclassified and did non have fatty liver on review were excluded (Effigy 1). A total of 175 patients were excluded for other reasons than based on histopathology (Figure 1). The remaining study group of 245 patients had no signs of viral hepatitis in the index liver biopsy and did non receive whatsoever medication known to be associated with the development of steatosis.
Medical records from these patients were traced and the biopsies reviewed by experienced pathologists. A total of 245 patients constituted the study group, 136 (56%) women and 109 men (44%). Women were in the majority in the NAFLD group, 105/151 (70%) compared to 46/151 (30%) men (p < 0.001). The proportion of men was higher in the AFLD group, that is 67% (63/94) whereas the proportion of women was 31/94 (33%).
Clinical and biochemical results
Clinical and biochemical information at the fourth dimension of index liver biopsy in the 245 patients of the two report groups (Table 1). Information was bachelor to calculate BMI in 56% of the total report cohort. No pregnant divergence was found in the BMI between the ii groups (Table 1). In the current context obesity was defined as BMI ≥ 30, 48/88 patients (55%) were obese in the NAFLD group compared to 22/50 patients (44%) in the AFLD group (NS). In the total cohort no meaning divergence was observed between the genders in terms of obesity as 31/76 (41%) of women were obese and 31/62 (fifty%) of the men and no difference was seen in BMI when comparing genders in the NAFLD and the AFLD group (data not shown). A total of 74/88 (84%), 52 women vs. 22 men in the NAFLD group had a BMI > 25 compared to 38/50 (76%), 9 women vs. 29 men in the AFLD grouping (NS).
The biochemical markers AST, ALT, bilirubin, prothrombin time and MCV were higher and platelets lower in the AFLD group compared to the NAFLD group at the time of index liver biopsy whereas other biochemical markers were similar in the two groups (Table i ). At the end of follow-up, ALT, AST and MCV were the just biochemical markers nonetheless significantly higher in the AFLD group compared to the NAFLD grouping (Table ane).
The clinical data on other diseases associated with the metabolic syndrome at the time of index liver biopsy and at the end of follow-upward catamenia in the two study groups are shown in Table two. The two groups had also similar morbidity in terms of atmospheric condition associated with metabolic syndrome both at baseline and at follow-upward (Tabular array 2). Overall, 58 (62%) of the patients in the AFLD grouping had undergone alcohol addiction therapy according to computerized database of patients in the National Middle of Addiction Medicine, whereas 2 (1%) in the NAFLD grouping had undergone an addiction therapy, not due to alcohol but due to abuse of sedatives and due to a gambling habit.
Histological cease-points and development of cirrhosis
The histological characteristics in the index liver biopsy are summarized in Table 3. Co-ordinate to the NAS score overall 31/151 (21%) patients in the NAFLD group had NASH compared to 35/94 (37%) with ASH in the AFLD grouping (p = 0.007). In the nonalcoholic grouping 47 (31%) patients had borderline NASH and 68 patients (45%) did non have steatohepatitis. In the alcoholic group 35 (37%) patients had deadline ASH (NS) and 22 (23%) did not have ASH (NS). Patients in the NAFLD had less astringent lobular inflammation than the AFLD group (Table three).
At the time of alphabetize liver biopsy xviii patients had cirrhosis, 6 patients in the NAFLD grouping and 12 in the AFLD group, respectively. Overall, eleven patients adult cirrhosis during follow-upward menstruum, four patients in the NAFLD group and seven patients in the AFLD group. Thus, a total of 29 patients were diagnosed with cirrhosis in the ii groups, 10 (7%) patients in the NAFLD group and 19 (20%) patients in the AFLD group (p = 0.003).
Amongst patients developing cirrhosis in the follow-upwardly period the histological diagnosis at baseline was as follow: one patient had no fibrosis (in the NAFLD group), three patients had stage 1A fibrosis (all three in the AFLD group), one patient had portal fibrosis (in the NAFLD group) and six patients bridging fibrosis (four in the AFLD grouping and two in the NAFLD grouping).
Liver-related complications
Patients developing liver cirrhosis and liver related complications are demonstrated in Tabular array iv. Among patients diagnosed with cirrhosis a somewhat higher proportion developed ascites in the AFLD group, xi/19 (58%) vs. NAFLD, 3/ten (30%) (p = 0.004). Only one patient in the AFLD group developed HCC but none of the NAFLD patients adult HCC (Table 4). A significantly higher number of patients in the AFLD group, xiii/94 (14%) developed decompensated liver disease compared with vii/151 (five%) in the NAFLD group (Tabular array iv). Information technology should be noted that baseline NAS score was dissimilar between two groups with higher baseline NAS score in the AFLD group (NAS score > 5: 37% vs 21%).
Survival and mortality
The median survival was 24.2 (range 0.2-26.1) years in the NAFLD grouping and 19.v (range 0.2-24.two) years in the AFLD group (p = 0.0007). Median follow-upwards time for the non-alcoholic grouping was ix.9 years (range 0.2-26 years) and 9.2 years (0.2-25 years) for the alcoholic group. In that location was no pregnant deviation in overall survival between the 2 study groups and no significant departure betwixt genders (data not shown). Patients in the AFLD group diagnosed with cirrhosis had a higher death rate compared to the NAFLD group; 10 patients (40%) in the AFLD grouping compared with 7 patients (17%) in the NAFLD grouping (NS). Using Cox assay the survival was significantly worse for patients in the AFLD group compared to the NAFLD grouping after adjusting for gender, calendar year of diagnosis and historic period at diagnosis (HR 2.16, p = 0.009) (Effigy 2). The hazard ratio for women in the AFLD group was ane.19 compared to the NAFDL group.The survival for patients with moderate to severe fibrosis was significantly worse than for patients with mild fibrosis after adjusting for gender, calendar year of diagnosis and age at diagnosis (HR 2.09, p = 0.01) (Effigy iii).
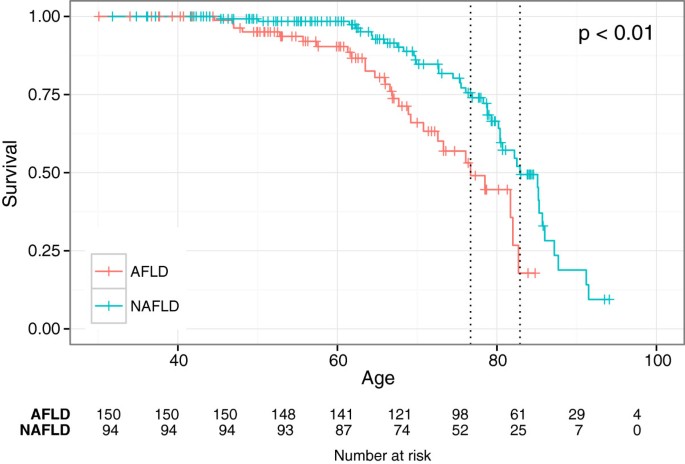
Kaplan Meier survival plots showing survival from day of nascency after correcting for historic period, gender and twelvemonth of diagnosis for the NAFLD- and AFLD groups. The light-green line showing the NAFLD (non-alcoholic fatty liver disease) group and the cerise line showing the AFLD (alcoholic fatty liver disease) group.
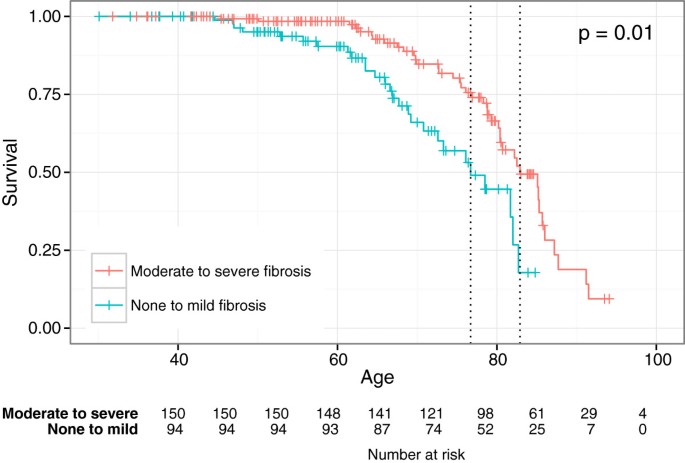
Kaplan Meier survival plots showing survival from day of birth after correcting for age, gender and twelvemonth of diagnosis for the none to mild fibrosis grouping (green line) and moderate to astringent fibrosis grouping (cherry-red line).
A total of 67 patients died during the follow-upwardly period; 41 women (61%) and 26 men (39%). Of these 12 (18%) were liver related in both the NAFLD and AFLD group (Table 5). The most common crusade of expiry was due to cardiovascular disease 28/67 (42%) followed past liver-related disease 12/67 (18%) and malignancy 12/67 (eighteen%) (Table five). 7% of deaths were liver-related in the NAFLD group, no human being in the NAFLD group died of liver-related disease whereas iii women had a liver-related death. In the AFLD group the most common cause of decease was liver-related, ix/25 (36%) followed by cardiovascular disease in 8/25 (32%) and malignancy among 6/25 (24%). The mean liver-related death rate among the general population during the study menses was 0.1% of all deaths [13]. In the AFLD group vi men and three women died of liver-related illness. Simply one patient died from hepatocellular cancer (HCC) in the total cohort and as mentioned above, from the AFLD grouping.
The most mutual cause of death in the NAFLD group was of cardiovascular affliction 20/42 (48%), followed by malignancy 6/42 (fourteen%) and other chronic medical atmospheric condition four/42 (9.5%). A total of 12 patients (18%) died of malignancy. In the AFLD group, iv died of breast cancer and one each of renal cancer, malignant encephalon tumor, colon cancer, nasopharyngeal cancer and pancreas cancer. In the NAFLD grouping, two died of chest cancer and ane each of prostate cancer, multiple myeloma, endometrial cancer and one of small cell lung cancer.
Discussion
Few studies have determined the natural history of biopsy-proven fatty liver disease and compared the long-term prognosis of these two major groups of fatty liver disease due to alcoholic and non-alcoholic fatty liver illness.
Our study has several methodological strengths. First, all patients had biopsy proven fatty liver disease and histology was re-evaluated based on validated scores. Nosotros believe nosotros have included the vast bulk of patients with biopsy-proven fatty liver disease in the whole population of Iceland during this catamenia every bit at least 95% of the population lives in the catchment expanse of the National Academy Hospital. The fact that all the patients underwent a liver biopsy is as well a weakness, especially when evaluating disease outcome. Previous studies have shown that NAFLD patients diagnosed with liver biopsy have a worse prognosis compared with patients diagnosed with ultrasonography. Therefore, studying patients recruited from the pathology registry involves a choice bias. It must be stressed that the indications for the liver biopsy was not e'er clear, although virtually cases were because of elevated liver function tests and/or hepatomegaly or suspected alcoholic liver affliction, and this in turn can give a selection bias. As well the indication for biopsy in NAFLD and AFLD may differ betwixt atmospheric condition and betwixt practitioners and might explain some of the differences in affliction consequence.
The main limitation of the study was its retrospective pattern and information was not systematically registrered and was therefore sometimes missing or unavailable. In improver the search for the code M-50080 (fatty liver) is limiting in itself as the more serious steatosis with fibrosis and even cirrhosis might be coded every bit something else than just fat liver. Since this was a retrospective study on liver biopsies it is not possible to standardize the size of the needle biopsies. Therefore the size is very variable and the range can exist considerable, but should be similar to the standards observed in pathology departments in general. Samples less than 2 mm in diameter would take been excluded from the study, but no such samples came into the study.
The slides used for pathological estimation were the original slides and recuts or restaining of slides was not done except for a few exceptional cases where the original slides were unavailable or when a Masson-Trichrome stain had not been performed originally. Occationally the colours of the slides had faided somewhat. This yet we do not anticipate having pregnant outcome on the results, especially since ballooning degeneration increases cell size and this is non greatly affected by fading colours.
Another limitation is the pocket-sized number of hard endpoints with only iv patients in the NAFLD group who developed cirrhosis over the follow-upwards period. There is also a potential incertitude in the non-histological diagnosis of cirrhosis which must exist taken into consideration when reviewing the results.
The information on ASH should be interpreted with circumspection every bit NAFLD activity score has to our knowledge not notwithstanding been validated in AFLD, but we chose to use information technology for comparison equally the histolopathological development is like in the two conditions and there is no deviation morphologically betwixt NAFLD and AFLD.
One of the main findings in this report was that patients with fat liver disease showed a markedly higher gamble of developing liver-related death compared to the general population. Although significantly higher in the AFLD grouping liver-related death in the NAFLD grouping was seven% of all deaths. These findings are in dissimilarity with liver-related expiry rate in Iceland [13] which was a mean of 0.1% in the full general population during the study period. As in other studies information technology is a claiming to classify patients into non-alcoholic and alcoholic group. We tried to minimize the misclassification by regrouping those without a known alcohol etiology if the patients were found to have an alcoholic related diagnosis later as for instance alcohol pancreatitis and alcohol dependence. In addition all patients were linked to the database for the National Centre of Addiction Medicine in Iceland.
Liver-related morbidity and mortality
Our results prove that patients with NAFLD had a rather benign form in terms of liver-related morbidity and bloodshed. Only vii% developed cirrhosis after a mean of xiii years of follow-up which is similiar to what previous studies on the prognosis of NAFLD have shown [half dozen, seven, 14–17]. A higher number of patients in the AFLD group developing cirrhosis (20%) after approximately 12 years of follow-upwards, is likewise in agreement with previous studies showing worse prognosis in patients with AFLD than NAFLD [8, 9, 18]. These studies have demonstrated that patients with alcoholic fatty liver disease have worse prognosis of their liver disease than patients with NAFLD [8, ix, 18]. In a written report on prognosis and life expectancy in chronic liver disease the 5 year survival was 38% for the alcoholic group and 68% for the non-alcoholic grouping but simply 87% of the patient underwent liver biopsy whereas the rest was diagnosed clinically or with ultrasound [xviii]. In another study of 7000 patients discharged with the diagnosis fatty liver the mortality was 5.4 fold amongst AFLD and 2.6 amongst NAFLD [19]. In the electric current study we constitute that the overall survival was worse in the AFLD group. Patients in the AFLD grouping had a higher liver-related mortality, but patients in the NAFLD group died more than oft from cardiovascular illness as already demonstrated in previous studies [6, 7, 14, xvi].
In the AFLD group the near common cause of death was liver-related (35%).
Other studies have shown that obesity in both NAFLD and AFLD predispose to the evolution of fatty liver and chronic liver illness [19, xx]. In Iceland, the prevalence of liver cirrhosis due to alcohol is very low, only 3.3/100.000 inhabitants which was 4 times lower than in Sweden [21]. In the current report 45% of the patients in the NAFLD grouping had a BMI ≥30 and somewhat surprisingly there was no pregnant difference in BMI between the NAFLD group and the AFLD grouping. The fact that patients with AFLD did non differ with respect to BMI and incidence of metabolic syndrome-related diseases might reverberate a mixed AFLD/NAFLD etiology in the alcoholic grouping. In the Dionysos study, obesity among heavy drinkers, increased the take chances for steatosis by twofold [19]. Moreover, no significant differences were evident concerning weather condition associated with metabolic syndrome neither at baseline nor at follow-up, but we had expected a higher portion of diseases associated with metabolic syndrome in the NAFLD group. In a study from Denmark, a significantly college BMI was seen in NAFLD than in AFLD patients. Withal, this might at to the lowest degree partly reflect the fact that their patients were recruited from an obesity research projection [8] whereas our patients were unselected patients undergoing a liver biopsy.
In the current study women were in the bulk in the NAFLD grouping but the high proportion of women with fatty liver compared to men may reflect a higher illness burden in women. A recent study from the U.s. as well found a higher proportion of women in the NAFLD group [22] which is in line with our results. A significantly higher prevalence of cirrhosis in female person AFLD patients was observed in a Danish written report and time to cirrhosis was associated with female gender [10]. Population based studies take shown increased risk of women developing booze-induced cirrhosis [23–26].
Progression of NAFLD has been plant to exist wearisome and seems to depend a great deal on the initial fibrosis stage [eight, 14]. Patients with simple fatty liver at baseline seem to take a good prognosis in terms of liver disease. In a Danish study of 109 patients diagnosed with pure non-alcoholic simple steatosis (without inflammation or significant fibrosis) only ane of the patients developed cirrhosis [eight]. In the current study more severe lobular inflammation was found in the AFLD grouping compared to the NAFLD group and a significantly college number of patients in the AFLD group had steatohepatitis compared to the NAFLD grouping.
In the total report cohort patients with more severe fibrosis at baseline showed a worse overall survival than patients with none or balmy fibrosis at baseline. Based on this nosotros were able to show an association in the total study accomplice between the phase of fibrosis and the prognosis. However more NAFLD than AFLD patients had mild or no fibrosis at baseline. This is in agreement with results from a contempo report showing that advanced fibrosis in the index liver biopsy was the nearly important predictor of the prognosis in these patients [27]. A contempo Danish study showed that the cirrhosis risk was more twice as loftier for the patients with steatohepatitis than for those with pure steatosis [26].
A Swedish cohort study of patients with biopsy-proven NAFLD and elevated liver tests showed that they had a similar survival compared to the Swedish population [seven]. Interestingly the risk of death was increased in patients with non-alcoholic steatohepatitis [7].
A study from Minnesota, identified 420 patients with NAFLD past imaging or liver biopsy found liver-related complications to be the tertiary most common cause of expiry among NAFLD patients [6]. This is similar to our results showing liver-related to exist the third most common cause of death amongst the NAFLD group. Still in the AFLD group liver-related death was the leading cause of death, followed by cardiovascular diseases and malignancy which is in accord to a previous study where hepatobiliary disease was the leading cause of death in the AFLD [9].
In the electric current study, no patient in the NAFLD group died of hepatocellular carcinoma and only one patient in the AFLD group. The absence of HCC among the NAFLD group differs from previous cohort studies showing that 3/129 (2%) [vii] and 2/420 (0.5%) [half dozen] of NAFLD patients developed HCC [vii]. A reasonable explanation for this divergence in our study could exist that our patients had in general mild changes in the liver biopsy at baseline. It is also conceivable that a longer follow-up time would probably lead to patients with HCC.
Cardiovascular disease
In agreement with many previous studies a markedly higher proportion of our women in the NAFLD group died of cardiovascular disease compared to women in the AFLD group, 17 patients vs. i patient respectively. A previous written report [10] showed that cardiovascular disease was the leading cause of decease in the AFLD group (men and women toghether), which is at odd with our results. In the current study the leading cause of decease in the AFLD group was liver related. We can non find a plausible caption for this deviation, although information technology has been shown that diagnoses on death certificates can underestimate liver-related bloodshed [28] which might have been the case in the Danish report [ten].
The most common cause of decease in the NAFLD grouping was from cardiovascular disease, followed by malignancy which is in agreement with findings of other cohort studies (6, 7, fourteen, 16,). I report plant 34% increased risk of cardiovascular mortality amid NAFLD patients compared to the general Minnesota population over a seven.6 year follow-up [six].
Conclusion
In determination a college proportion of patients with AFLD adult liver cirrhosis and had liver-related death compared to patients with NAFLD in this population based setting and had as well more severe histological changes in the liver biopsy at baseline. Patients in the AFLD group showed a significantly worse survival compared to patients in the NAFLD group. Patients with more severe fibrosis at baseline showed a worse survival than patients with none or balmy fibrosis at baseline. Patients with fat liver illness showed a markedly college risk of developing liver-related expiry compared to the full general population.
Abbreviations
- NAFLD:
-
Nonalcoholic fatty liver affliction
- AFLD:
-
Alcoholic fat liver disease
- HR:
-
Hazard ratio
- SNOMED:
-
Systemized nomenclature of medicine
- NUH:
-
National university infirmary
- RCD:
-
Registry of causes of death
- PAS:
-
Periodic acrid schiff
- ALT:
-
Alanine aminotransaminase
- AST:
-
Aspartate aminotransferase
- ALP:
-
Alkaline phosphatase
- PT:
-
Prothrombin time
- PLT:
-
Platelets count
- TG:
-
Triglycerides
- MCV:
-
Mean corpuscular volume
- NS:
-
Not significant
- NASH:
-
Non-alcoholic steatohepatitis
- ASH:
-
Alcoholic steatohepatitis
- NAS:
-
Non-alcoholic fat liver disease activity score
- HCC:
-
Hepatocellular carcinoma
- BMI:
-
Trunk mass index.
References
-
Bellantini S, Scaglioni F, Marino M, Bedogni Thou: Epidemiology of non-alcoholic fat liver disease. Dig Dis. 2010, 28: 155-161.
-
Lazo M, Clark JM: The epidemiology of nonalcoholic fatty liver affliction: a global perspective. Semin Liver Dis. 2008, 28: 339-350.
-
Angulo P: Nonalcoholic fatty liver disease. Northward Engl J Med. 2002, 346: 1221-1231.
-
Friis-Liby I, Aldenborg F, Jerlstad P, Rundström K, Björnsson E: High prevalence of metabolic complications in patients with non-alcoholic fatty liver disease. Scand J Gastroenterol. 2004, 39: 864-869.
-
Day PC: Not-alcoholic steatohepatitis (NASH): where are we now and where are we going. Gut. 2002, 50: 585-
-
Adams LA, Lymp JF, St. Sauver J, Sanderson SO, Lindor KD, Feldstein A, Angulo P: The natural history of nonalcoholic fatty liver disease: a population-based cohort study. Gastroenterology. 2005, 129: 113-121.
-
Ekstedt M, Franzén LE, Mathiesen UL, Thorelius L, Holmqvist G, Bodemar Yard, Kechagias Due south: Long-term follow-up of patients with NAFLD and elevated liver enzymes. Hepatology. 2006, 44: 865-873.
-
Dam-Larsen S, Franzmann M, Andersen IB, Christoffersen P, Jensen LB, Sörensen TIA, Becker U, Bendtsen F: Long term prognosis of fatty liver: gamble of chronic liver disease and death. Gut. 2004, 53: 750-755.
-
Jepsen P, Vilstrup H, Mellemkjær 50, Thulstrup AM, Olsen JH, Businesswoman JA, Sörensen HT: Prognosis of patients with a diagnosis of fatty liver – a registry-based cohort report. Hepato-Gastroenterology. 2003, l: 2101-2104.
-
Dam-Larsen S, Becker U, Franzmann MB, Larsen K, Christoffersen P, Bendtsen F: Final results of long-term, clinical follow-upward in fatty liver patients. Scand J Gastroenterol. 2009, 44: 1236-1243.
-
Kleiner DE, Brunt EM, Van Natta M, Behling C, Contos MJ, Cummings OW, Ferrell LD, Liu YC, Torbenson MS, Unalp-Arida A, Yeh M, McCullough AJ, Sanyal AJ: Design and validation of a histological scoring organisation for nonalcoholic fatty liver disease. Hepatology. 2005, 41: 1313-1321.
-
Burden EM, Janney CG, Di Bisceglie AM, Neuschwander-Tetri BA, Bacon BR: Nonalcoholic steatohepatitis: a proposal for grading and staging the histological lesions. Am J Gastroenterol. 1999, 94: 2467-2474.
-
Statistics Iceland: 2013, Bachelor from: http://www.hagstofan.is/Hagtolur/Mannfjoldi/faeddir-og-danir
-
Matteoni CA, Younossi ZM, Gramlich T, Boparai N, Liu YC, McCullough AJ: Nonalcoholic fat liver disease. A spectrum of clinical and pathological severity. Gastroenterology. 1999, 116: 1413-1419.
-
Ong JP, Pitts A, Younossi ZM: Increased overall bloodshed and liver-related bloodshed in not-alcoholic fatty liver disease. J Hepatol. 2008, 49: 608-612.
-
Söderberg C, Stål P, Askling J, Glaumann H, Lindberg Grand, Marmur J, Hultcrantz R: Decreased survival of subjects with elevated liver function tests during a 28-year old follow up. Hepatology. 2010, 51: 595-602.
-
Lee GR: Nonalcoholic steatohepatitis: a written report of 49 patients. Hum Pathol. 1989, 20: 594-
-
Propst A, Propst T, Zangerl M, Ofner D, Judmaier Grand, Vogel W: Prognosis and life expectancy in chronic liver disease. Dig Dis Sci. 1995, forty: 1805-1815.
-
Bellantini S, Saccoccio Yard, Masutti F, Croce LS, Brandi G, Sasso F, Cristanini Thousand, Tiribelli C: Prevalence of and hazard factors for hepatic steatosis in Northern Italy. Ann Intern Med. 2000, 132: 112-117.
-
Naveau South, Giraud V, Borotto E, Aubert A, Capron F, Chaput J: Excess weight risk cistron for alcoholic liver illness. Hepatology. 1997, 25: 108-111.
-
Gunnarsdottir SA, Olsson R, Olafsson Due south, Cariglia N, Westin J, Thjodleifsson B, Björnsson E: Liver cirrhosis in Republic of iceland and Sweden: incidence, aetiology and outcomes. Scand J Gastroenterol. 2009, 44: 984-993.
-
Neuschwander-Tetri BA, Clark JM, Bass NM, Van Natta M, Unalp-Arida A, Tonascia J, Zein CO, Brunt EM, Kleiner DE, McCullough AJ, Sanyal AJ, Diehl AM, Lavine JE, Chalasani N, Kowdley KV: Clinical, laboratory and histological associations in adults with nonalcoholic fatty liver disease. Hepatology. 2010, 52: 913-924.
-
Klatsky AL, Armstrong MA, Friedman GD: Booze and mortality. Ann Intern Med. 1992, 117: 646-654.
-
Becker U, Deis A, Sorensen TIA, Borch-Johnsen K, Muller CF, Schnohr P, Jensen One thousand: Prediction of risk of liver illness by alcohol intake, sex activity, and historic period: a prospective population report. Hepatology. 1996, 23: 1025-1029.
-
Kamper-Jorgensen K, Gronbaek One thousand, Tolstrup J, Becker U: Alcohol and cirrhosis: dose–response or threshold issue?. J Hepatology. 2004, 41: 25-30.
-
Deleuran T, Grønbæk H, Vilstrup H, Jepsen P: Cirrhosis and mortality risks of biopsy-verified alcoholic pure steatosis and steatohepatitis: a nationwide registry-based study. Aliment Pharmacol Ther. 2012, 35: 1336-
-
Angulo P, Bugianesi East, Björnsson Due east, Charatcharoenwitthaya P, Mills PR, Barrera F, Haflidadottir Southward, Solar day CS: Uncomplicated non-invasive systems predict long-term outcomes in patients with nonalcoholic fat liver disease. Gastroenterology. 2013, 145: 782-789.
-
Prytz H, Skinhoj P: Morbidity, bloodshed, and incidence of cirrhosis in Kingdom of denmark 1976–1978. Browse J Gastroent. 1981, 16: 839-844.
Pre-publication history
-
The pre-publication history for this paper tin can be accessed here:http://www.biomedcentral.com/1471-230X/14/166/prepub
Acknowledgments
Funding Acknowledgement: This research was supported in part past the Intramural Enquiry Program of the NIH, National Cancer Plant. Study was also supported by the Academy Hospital of Iceland Inquiry Fund.
Author information
Affiliations
Corresponding author
Boosted data
Competing interests
The authors declare that they take no competing interests.
Authors' contribution
SH conceived and designed the report, acquired data, critically analyzed the results and drafted the article, JGJ analyzed and scored the liver biopsies and contributed to the data give-and-take, HN acquired data and contributed to the data give-and-take, SOE analyzed and scored the liver biopsies, DEK analyzed and scored the liver biopsies and contributed to the data discussion, SHL performed the statistical analysis, ESB conceived and designed the study, contributed to the data discussion and participated in its coordination. All authors read and approved the concluding manuscript.
Authors' original submitted files for images
Rights and permissions
Open Admission This commodity is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, every bit long every bit y'all give appropriate credit to the original author(due south) and the source, provide a link to the Creative Commons licence, and indicate if changes were made.
The images or other third party material in this article are included in the article'southward Creative Commons licence, unless indicated otherwise in a credit line to the cloth. If fabric is not included in the article's Creative Commons licence and your intended utilize is non permitted by statutory regulation or exceeds the permitted use, you will demand to obtain permission direct from the copyright holder.
To view a copy of this licence, visit https://creativecommons.org/licenses/by/4.0/.
The Creative Commons Public Domain Dedication waiver (https://creativecommons.org/publicdomain/null/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the information.
Reprints and Permissions
Near this commodity
Cite this article
Haflidadottir, S., Jonasson, J.G., Norland, H. et al. Long term follow-upwards and liver-related expiry rate in patients with not-alcoholic and alcoholic related fatty liver affliction. BMC Gastroenterol 14, 166 (2014). https://doi.org/ten.1186/1471-230X-14-166
-
Received:
-
Accustomed:
-
Published:
-
DOI : https://doi.org/10.1186/1471-230X-fourteen-166
Keywords
- NAFLD
- AFLD
- Fibrosis
- Prognosis
- Mortality
Source: https://bmcgastroenterol.biomedcentral.com/articles/10.1186/1471-230X-14-166
0 Response to "How Long Can You Live With a Fatty Liver"
Post a Comment